Running Head: State and Insurance Type Variation in COPD
Funding Support: This study was funded by AstraZeneca Pharmaceuticals LP (Wilmington, Delaware). Milliman, Inc., received consulting fees from AstraZeneca Pharmaceuticals LP to conduct the research and provide editorial support for the manuscript.
Date of Acceptance: February 26, 2025 | Publication Online Date:
Abbreviations: AHA=American Hospital Association; BRFSS=Behavioral Risk Factor Surveillance System; C=commercial; CMS=Centers for Medicare & Medicaid Services; COPD=chronic obstructive pulmonary disease; ED=emergency department; ED/Obs=emergency department/observation; FFS=fee-for-service; GOLD=Global initiative for chronic Obstructive Lung Disease; HCG=Milliman Consolidated Health Cost Guidelines™; HCPCS=Healthcare Common Procedure Coding System; HCUP=Healthcare Cost and Utilization Project; ICD-10-CM=International Classification of Diseases, Tenth Revision, Clinical Modification; LABA=long-acting beta2-agonist; LAMA=long-acting muscarinic antagonist; MC=Medicare; MD=Medicaid; T-MSIS=Transformed Medicaid Statistical Information System
Citation: Bazell C, Alston M, Feigler N, et al. Variation in prevalence and burden of chronic obstructive pulmonary disease by state and insurance type in the United States. Chronic Obstr Pulm Dis. 2025; 12(2): 158-174. doi: http://doi.org/10.15326/jcopdf.2024.0560
Online Supplemental Material: Read Online Supplemental Material (1245KB)
Introduction
Chronic obstructive pulmonary disease (COPD) is a heterogeneous lung condition characterized by chronic respiratory symptoms caused by abnormalities of the airways and alveoli that result in persistent, often progressive, airflow obstruction.1 This condition poses a significant challenge to the individuals living with COPD and the health care system due to its prevalence, impact on health and quality of life, and contribution to mortality. Chronic lower respiratory disease (including COPD) was the sixth leading cause of death2 in the United States in 2018–2021, and 10.1% of adults aged 45 and older have COPD based on 2021 Behavioral Risk Factor Surveillance System (BRFSS) survey data.3 State-level prevalence varies substantially, with the highest rate seen in West Virginia (17.3%) and the lowest reported in Hawaii (6.0%).3
Known risk factors for developing COPD include environmental exposures such as: tobacco smoking4; inhalation of toxic particles and gases from household5 and outdoor air pollution6; occupational exposures such as pesticides7 and burn pits8; infections such as human immunodeficiency virus infection9 and tuberculosis10; other medical conditions such as asthma11; and increasing age.12 Furthermore, low socioeconomic status is associated with an elevated lifetime risk of developing COPD.13
COPD poses a substantial burden on individuals with COPD and the health care system,14,15 with direct costs generally increasing with COPD severity and exacerbation frequency.16 Acute hospital-based health care utilization related to COPD is not uniformly distributed nationwide, and previous analysis found wide variation in COPD hospitalizations and emergency department (ED) visits among states.3
While there is recent information on COPD prevalence at the national and state levels from survey data and COPD-related acute hospital-based utilization from public health tracking sources, there is no current, comprehensive information available describing individuals living with COPD and their hospital-based health care utilization at the state level and by type of insurance coverage. Health insurance coverage in the United States falls under 2 main categories: public coverage (provided by the Medicare and Medicaid programs) and private coverage or commercial insurance (e.g., employment-based and direct purchase insurance plans).17 Medicare provides health insurance for individuals aged 65 years or older and individuals under 65 with certain medical conditions or disabilities18; and Medicaid provides health insurance for eligible children, pregnant women, adults with limited income, and elderly or disabled adults.19
Because states design and administer their own Medicaid programs within federal rules20 and differ in their decisions on the Affordable Care Act’s expansion of Medicaid coverage,21 the characteristics and health of the Medicaid-insured population differ substantially by state. In contrast, Medicare has nationally consistent eligibility criteria that result in more similar populations of Medicare-insured individuals across states. Commercial insurance is primarily provided through employment but the availability of payers operating across local individual health insurance exchanges varies, which can result in heterogenous commercial insurance enrollment across states.22
The varying health insurance eligibility requirements and resulting mix of insurance coverages across states have potential implications for COPD prevalence and COPD-related acute hospital-based utilization identified from administrative claims. For example, smoking tobacco is a well-established risk factor for COPD and COPD exacerbations.23 Medicaid-insured individuals, who have the highest cigarette smoking rates,24 also have the highest 30-day hospital readmission rates following COPD-related hospitalizations.25 Additionally, the older Medicare population has both higher prevalence and complexity of COPD, based on the occurrence of claims for certain comorbid conditions, compared to the younger commercially-insured population, consistent with increasing age as a COPD risk factor.26
The objective of this study is to characterize the diagnosed population with COPD and their COPD-related acute hospital-based utilization and all-cause mortality among the U.S. insured population by insurance type and state (“state” in this paper includes states, Puerto Rico, and the District of Columbia). This information may provide insights into opportunities for reducing the substantial burden of COPD on individuals and the health care system.
Methods
Study Design
This observational retrospective study used the 2019–2021 Medicare 100% Research Identifiable Files, which contain all Medicare Parts A, B, and D claims data for 100% of Medicare fee-for-service (FFS)-insured individuals; the 2019–2021 (preliminary for 2021) Transformed Medicaid Statistical Information System (T-MSIS) Analytic Files, which contain all claims data (Medicaid FFS) and encounter data (managed Medicaid) for 100% of Medicaid-insured individuals; and the 2019–2021 Milliman Consolidated Health Cost Guidelines™ (HCG) Sources Database+ Analytic Files, which contain claims data for approximately 50 million (23% of) commercially-insured individuals. Medical and pharmacy administrative claims were used to identify individuals diagnosed with COPD between January 1, 2019, and December 31, 2021. Demographics and outcome metrics were identified from January 1, 2021, through December 31, 2021 medical and pharmacy claims.
Insured COPD Sample Populations
Insured Population
Individuals were included in the insured population samples if they met all of the following inclusion criteria in 2021: (1) had at least one month of medical and pharmacy enrollment, (2) had both medical and pharmacy coverage for each enrollment month, (3) were continuously enrolled from the first month of enrollment (i.e., no gap in coverage) through all months of coverage, and (4) were at least 40 years of age. All individuals covered by Medicare and Medicaid were included in the Medicare population and excluded from the Medicaid population. Individuals were assigned to states using mailing address locations. All references to insured individuals or the insured population throughout this paper mean individuals insured by Medicaid, Medicare, or commercial health insurance.
COPD Sample Population
Individuals in the insured population samples were identified as diagnosed with COPD if they met at least one of the following criteria between January 1, 2019, and December 31, 2021: (1) at least one acute or nonacute inpatient claim (Table B1 in the online supplement) with a COPD International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) diagnosis code (Table B2 in the online supplement) reported in any diagnosis code position; and (2) at least 2 qualified outpatient, emergency department (ED), observation, or urgent care claims (Table B1 in the online supplement) with a COPD ICD-10-CM diagnosis code (Table B2 in the online supplement) reported in any diagnosis code position on different dates of service at least 30 days apart.
Exclusion Criteria
Commercially-insured individuals diagnosed with COPD aged 65 or older in 2021 were excluded to avoid member duplication due to universal eligibility for age-based Medicare coverage that begins at age 65.
COPD Prevalence Estimation
See Figure A1 in the online supplement for the development of the COPD population samples for each insurance type. Due to data quality limitations, prevalence metrics for Puerto Rico and the District of Columbia for Medicaid and commercial insurance were replaced with the South Atlantic census division values.
COPD Sample Population Extrapolation
To extrapolate insured individuals with COPD from the sample populations identified in claims data to the total insured COPD populations, insurance type-specific COPD prevalence rates at the state and nationwide geographic levels were multiplied by the total insured population counts for each insurance type at the corresponding geographic levels. Total insured population counts were sourced from Centers for Medicare & Medicaid Services (CMS) data,27 T-MSIS enrollment files, and the American Community Survey28 and Small Area Health Insurance Estimates29 data, for Medicare, Medicaid, and commercial insurance types respectively. Medicare FFS COPD prevalence rates were used to extrapolate to all of Medicare (FFS and Medicare Advantage). Outcome metric rates were determined from claims data for the COPD sample populations as rates per 1000 individuals with COPD in each insurance type and geography and multiplied by the total insured COPD population count for each insurance type and level of geography as described above.
COPD Sample Population Demographics
Sample population demographic metrics were assigned to states based on the mailing address location of individuals with COPD. Due to data quality limitations, demographic metrics for Puerto Rico and the District of Columbia for Medicaid and commercial insurance were replaced with the South Atlantic census division values.
Age
Age refers to an individual’s age as of January 1, 2021, using date of birth for Medicare and Medicaid-insured populations and year of birth for the commercially-insured population.
Dual Eligibility
Medicare-insured individuals were identified as dually eligible if they had at least one month of dual-eligibility in 2021 based on the combination of monthly Medicare-Medicaid dual-eligibility code and Medicare entitlement/buy-in indicator in Medicare data.
Sample Population Outcome Metrics
Sample population outcome metrics were assigned to states based on the mailing address location of individuals with COPD who experienced the outcomes. The number of COPD-related hospitalizations and 30-day readmissions in Medicare, Medicaid, and commercial claims data were extrapolated to the total hospitalization and readmission counts using the same methodology described in the COPD Sample Population Extrapolation section. Due to data quality limitations, the same adjustments described in the COPD Sample Population Extrapolation section were applied. Additionally, the commercial insurance readmission rate for Montana was replaced with the Mountain census division value due to low sample size.
All-Cause Mortality
All-cause mortality was identified for individuals with COPD who had a date of death from any cause in 2021. Mortality information was only available for Medicare- and Medicaid-insured individuals.
COPD-Related Acute Hospital-Based Utilization
COPD-related acute hospital-based utilization was defined as hospital-based utilization (inpatient hospitalizations and emergency department/observation encounters) that met at least one of the following criteria: (1) a principal diagnosis code of COPD (Table B2 in the online supplement); (2) a principal diagnosis code of an acute pulmonary condition, sepsis, or respiratory failure (Table B3 in the online supplement), and a secondary diagnosis code of COPD unless the principal diagnosis code was for select acute pulmonary conditions commonly diagnosed in the setting of COPD exacerbations, such as acute bronchitis and unspecified pneumonia (Table B3 in the online supplement); or (3) a specific diagnosis code for COPD or bronchiectasis with acute lower respiratory infection or acute exacerbation in any diagnosis code position (acute exacerbations in Tables B2 and B3 in the online supplement).
COPD-Related Acute Inpatient Hospitalizations
COPD-related acute inpatient hospitalizations were identified from acute inpatient hospital facility claims that met the COPD-related acute hospital-based utilization definition above. Acute inpatient facility claims were identified from specific claim files (Medicare, Medicaid), provider numbers (Medicare), and claims characteristics, including bill types and revenue codes (Medicaid, commercial).
COPD-Related Emergency Department/Observation Encounters
COPD-related emergency department/observation (ED/Obs) encounters were identified from outpatient facility claims for emergency department and observation encounters at a hospital that met the COPD-related acute hospital-based utilization definition above but which did not result in an acute inpatient admission to that hospital.
Outpatient facility claims for ED/Obs encounters for Medicare- and commercially-insured individuals were identified from specific claim files, bill types, provider specialty codes, and/or ED-specific revenue and HCPCS codes. For Medicaid-insured individuals, identification of outpatient facility claims for ED/Obs encounters for 36 states and Puerto Rico was based on CMS’ recommended approach, which utilizes a combination of place-of-service, bill type, and revenue codes to identify outpatient institutional claims,30 coupled with ED-specific revenue codes and ED and observation HCPCS codes. For 12 states that had data quality issues impacting at least one of the CMS methodology’s characteristics for identifying outpatient facility claims, or where this standard approach resulted in noncredible values, approaches using other combinations of these characteristics were used. For Utah, Illinois, and the District of Columbia, no standard characteristics used in CMS’ methodology were supported by usable data so the COPD-related ED/Obs utilization metrics were replaced with the respective census division values for each state for Medicaid.
30-day Readmission Rates Following COPD-Related Acute Inpatient Hospitalizations
Readmissions were unplanned admissions to an acute inpatient hospital that occurred within 30 days following discharge from a COPD-related acute inpatient hospitalization (index admission). Readmissions were considered “planned” and excluded if they were for certain types of care (e.g., transplant surgery) or for scheduled procedures not resulting in acute illness or complications of care.31 Index admissions were excluded if they met at least one the following criteria: (1) the individual was not discharged alive, (2) the individual did not have 30 days postdischarge enrollment, or (3) the individual was discharged against medical advice. Only the first admission within 30 days of the index admission’s discharge date was considered a readmission, and readmissions to the same hospital on the day of discharge and for the same condition as the index admission were considered a single admission.
Results
Prevalence and Demographic Characteristics
Figure 1 displays the prevalence and insurance type distribution of insured individuals with COPD by state. COPD prevalence was highly variable, with Utah having the lowest rate (44 per 1000 insured individuals) and West Virginia having the highest (143 per 1000 insured individuals). Across all states, Medicare covered the highest proportion of insured individuals with COPD. See Table A1 in the online supplement for prevalence and count of individuals with COPD for each insurance type and state.
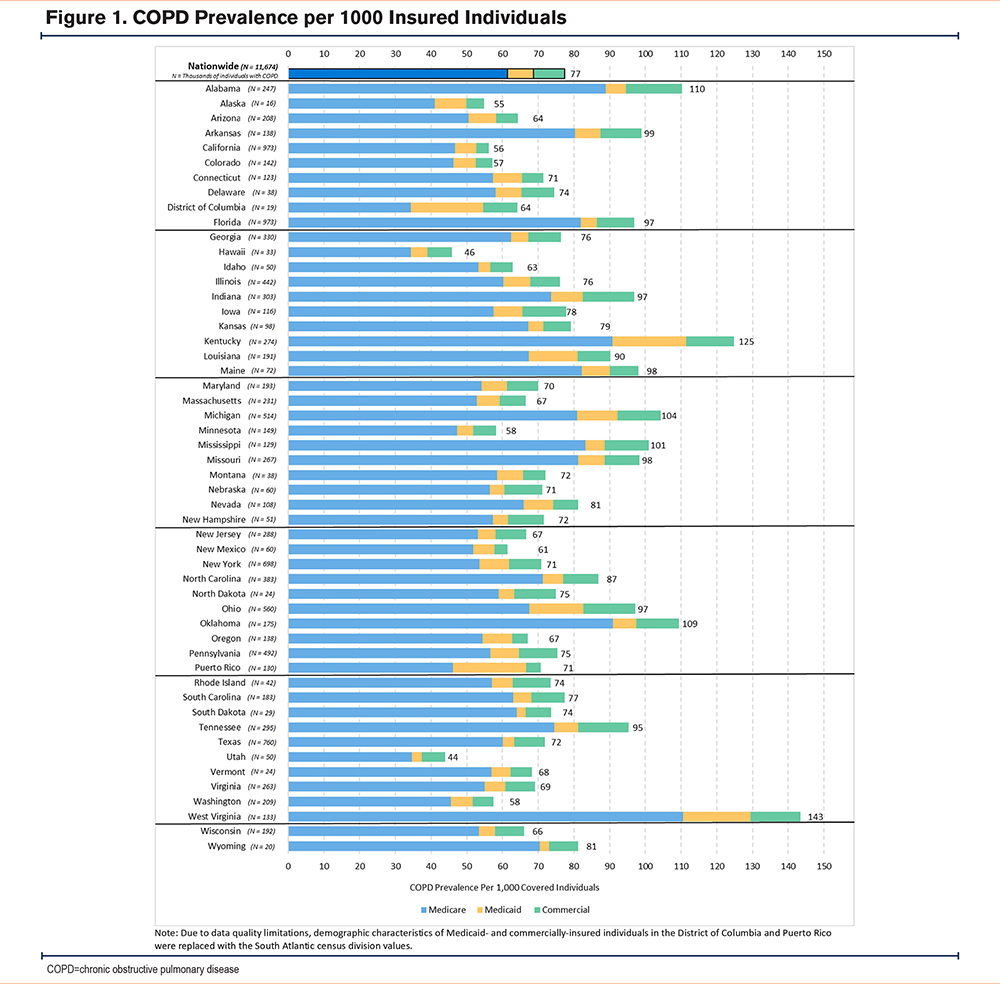
Figure 2 displays the prevalence of COPD among Medicaid-insured individuals compared to the Medicaid proportion of total non-Medicare-insured individuals (Medicaid- and commercial-insured individuals aged 40–64) in each state. While Medicaid insured a relatively low proportion of the non-Medicare-insured population aged 40–64 in non-expansion states, COPD prevalence was relatively high in Medicaid-insured individuals.
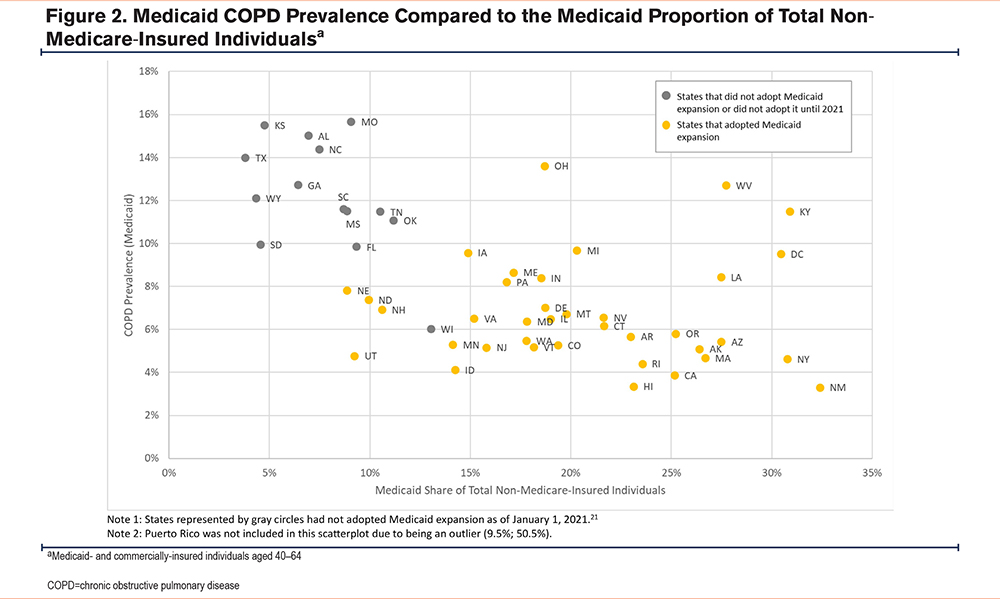
Table 1 displays demographic characteristics of insured individuals with COPD, by state and insurance type. Individuals with COPD insured by Medicare—including those who were dually eligible for Medicaid—were the oldest with a mean age of 73 years, compared to Medicaid (55 years) and commercial (56 years). The majority of individuals with COPD were female in all states except Hawaii. All-cause mortality rates were higher among individuals with COPD insured by Medicare compared to those insured by Medicaid at 11.5% and 5.1%, respectively.
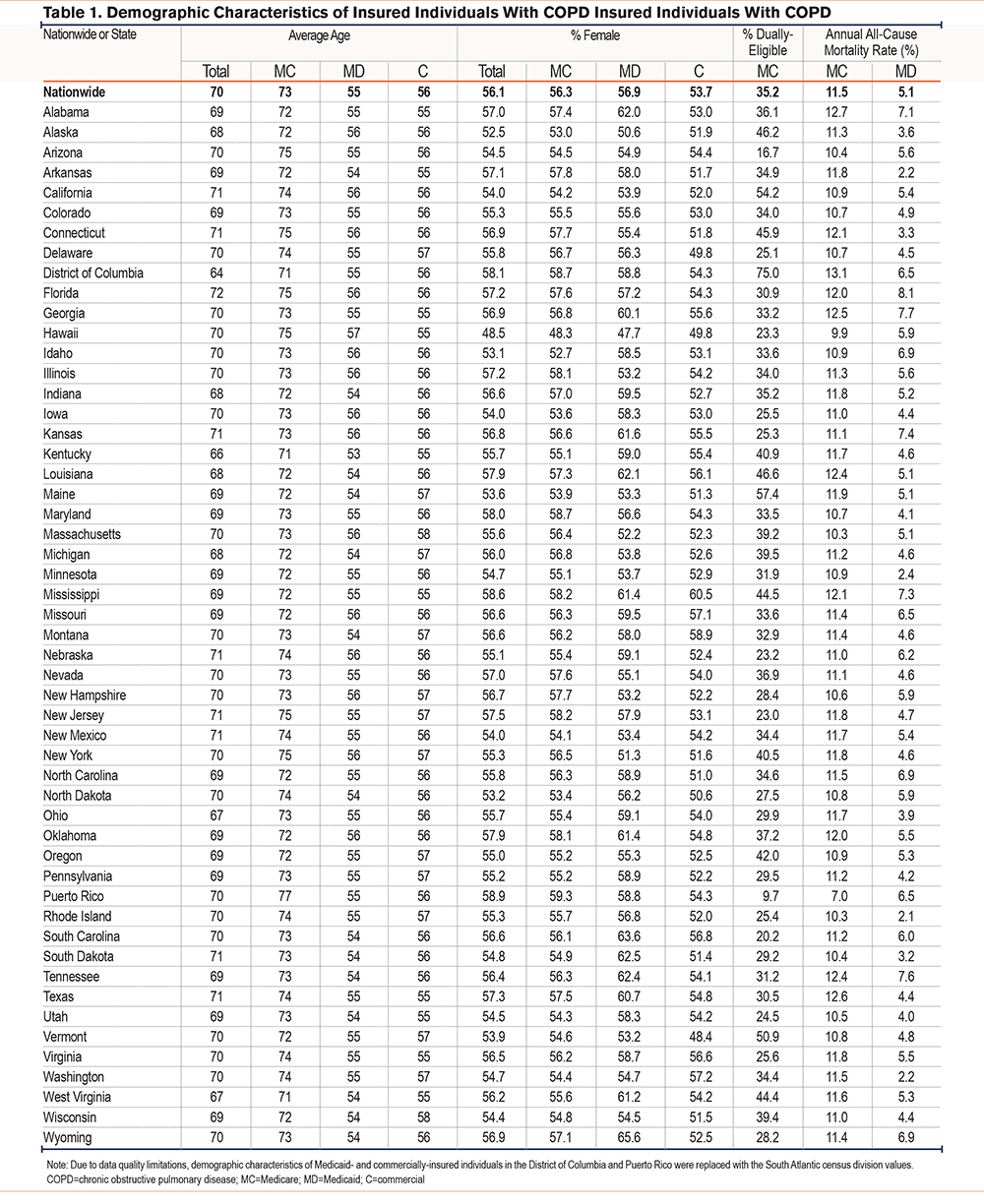
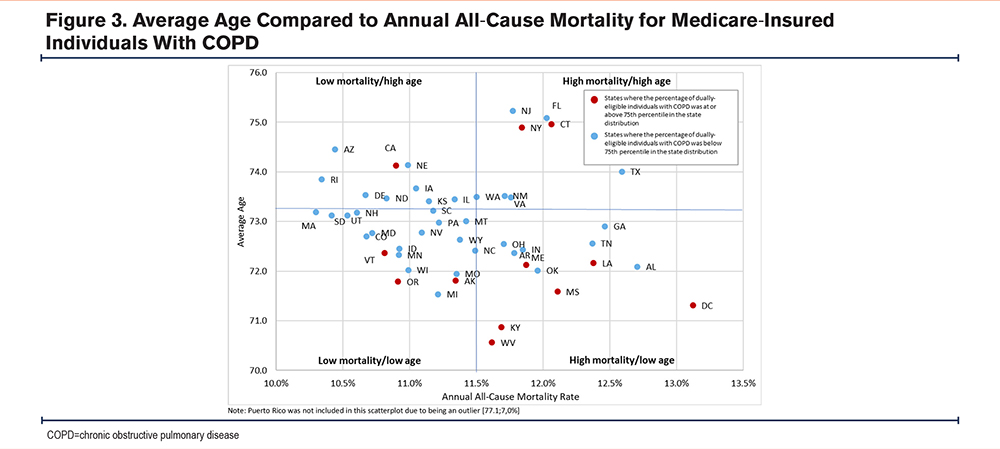
Figure 3 displays a comparison of the average age of individuals with COPD insured by Medicare and the annual all-cause mortality rate for that population. The vertical (age) and horizontal (all-cause mortality) lines, which indicate the national average for the respective metric, divide the chart into 4 quadrants. Almost half (46.2%) of the states in the high mortality/low age quadrant had a high percentage (above the 75th percentile in the state distribution) of dually eligible Medicare-insured individuals with COPD compared to other states with different mortality/age relationships, where all-cause mortality was consistent with or lower than age-based expectations. Among states in the high mortality/low age quadrant, all-cause mortality was higher than would generally be expected based on age. Figure A2 in the online supplement shows that all states (except Puerto Rico) had a higher percentage of individuals with COPD covered by Medicare who were dually eligible compared to the percentage of all Medicare-covered individuals who were dually eligible.
COPD-Related Acute Inpatient Hospitalizations
Figure 4 displays the rates and insurance type distribution of COPD-related acute inpatient hospitalizations for insured individuals with COPD by state. Nationwide, there were 154 COPD-related acute inpatient hospitalizations per 1000 insured individuals with COPD. This figure shows the variation and substantial national burden of COPD-related acute inpatient hospitalizations, with Idaho having the lowest rate (97 per 1000) and the District of Columbia having the highest (200 per 1000). Medicare covered the highest proportion (65.8%–92.5%) of COPD-related acute inpatient hospitalizations in each state except for Puerto Rico, where Medicaid’s share was highest (49.6%).
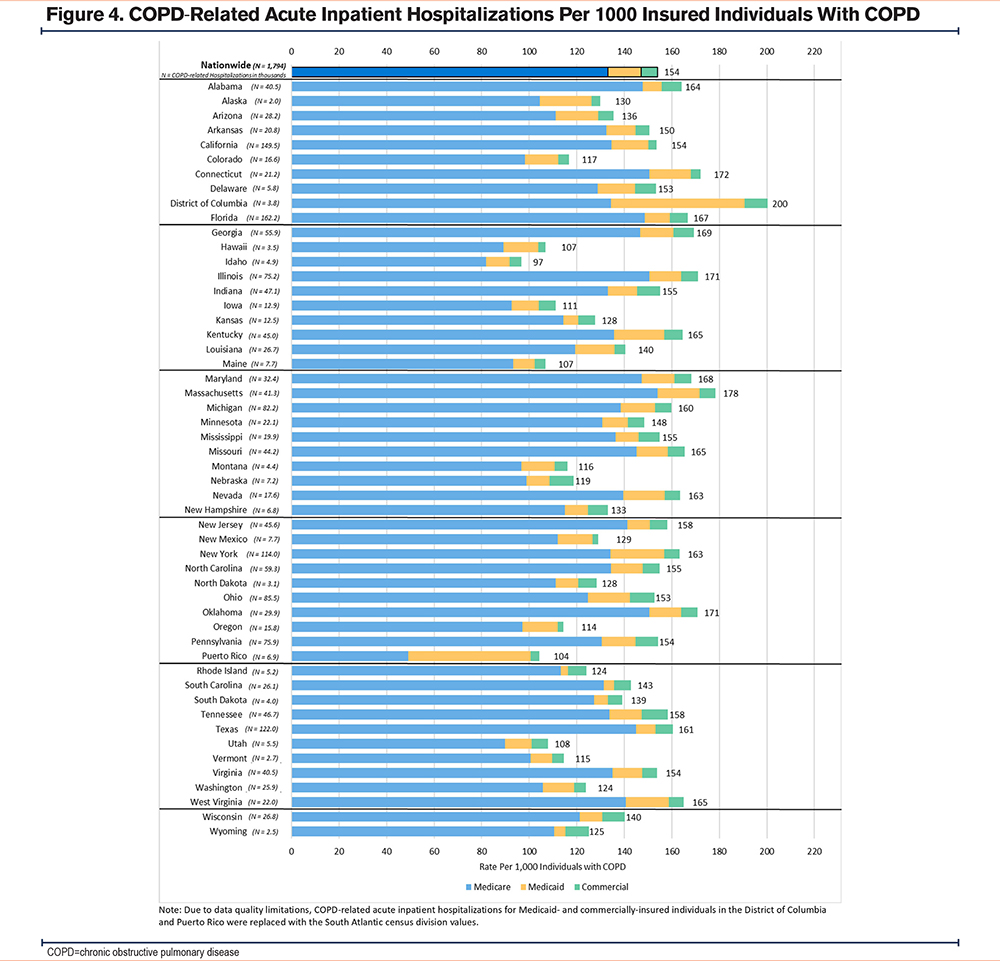
Figure 5 displays the percentage of insured individuals with COPD who had at least one COPD-related acute inpatient hospitalization by insurance type and state. Nationwide and in most states, a similar percentage of Medicare-insured individuals with COPD had at least one COPD-related acute inpatient hospitalization compared to Medicaid-insured individuals (12.2% versus 12.0% nationwide). The percentage of commercially-insured individuals with COPD with at least one COPD-related acute inpatient admission (5.2% nationwide) was less than half that of Medicare-insured individuals nationwide and across most states.
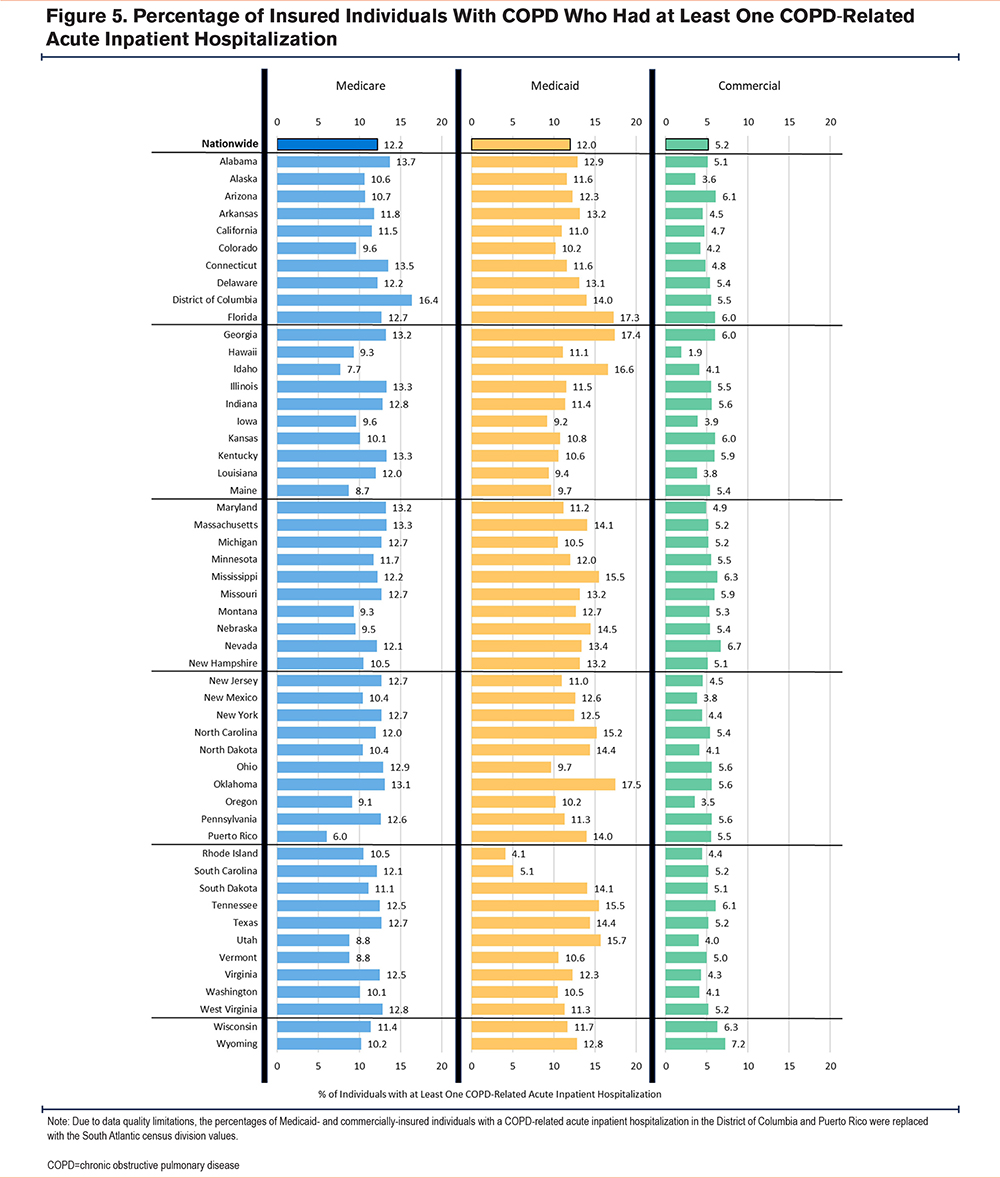
Table 2 displays COPD-related acute inpatient hospitalization metrics for insured individuals with COPD by state and insurance type. Nationwide, there were approximately 1.8 million COPD-related acute inpatient hospitalizations among insured individuals in 2021, and 11.4% of insured individuals with COPD had at least one COPD-related acute inpatient hospitalization. Medicare accounted for 86.4% of these hospitalizations, while Medicaid and commercial insurance accounted for 9.0% and 4.6%, respectively. About 20.4% of COPD-related acute inpatient hospitalizations resulted in an all-cause readmission within 30 days after discharge. Information on ED/Obs encounters for insured individuals with COPD is reported in Table A2 in the online supplement and shows 1.4 million COPD-related ED/Obs encounters among insured individuals nationwide, with rates varying among states and insurance types.
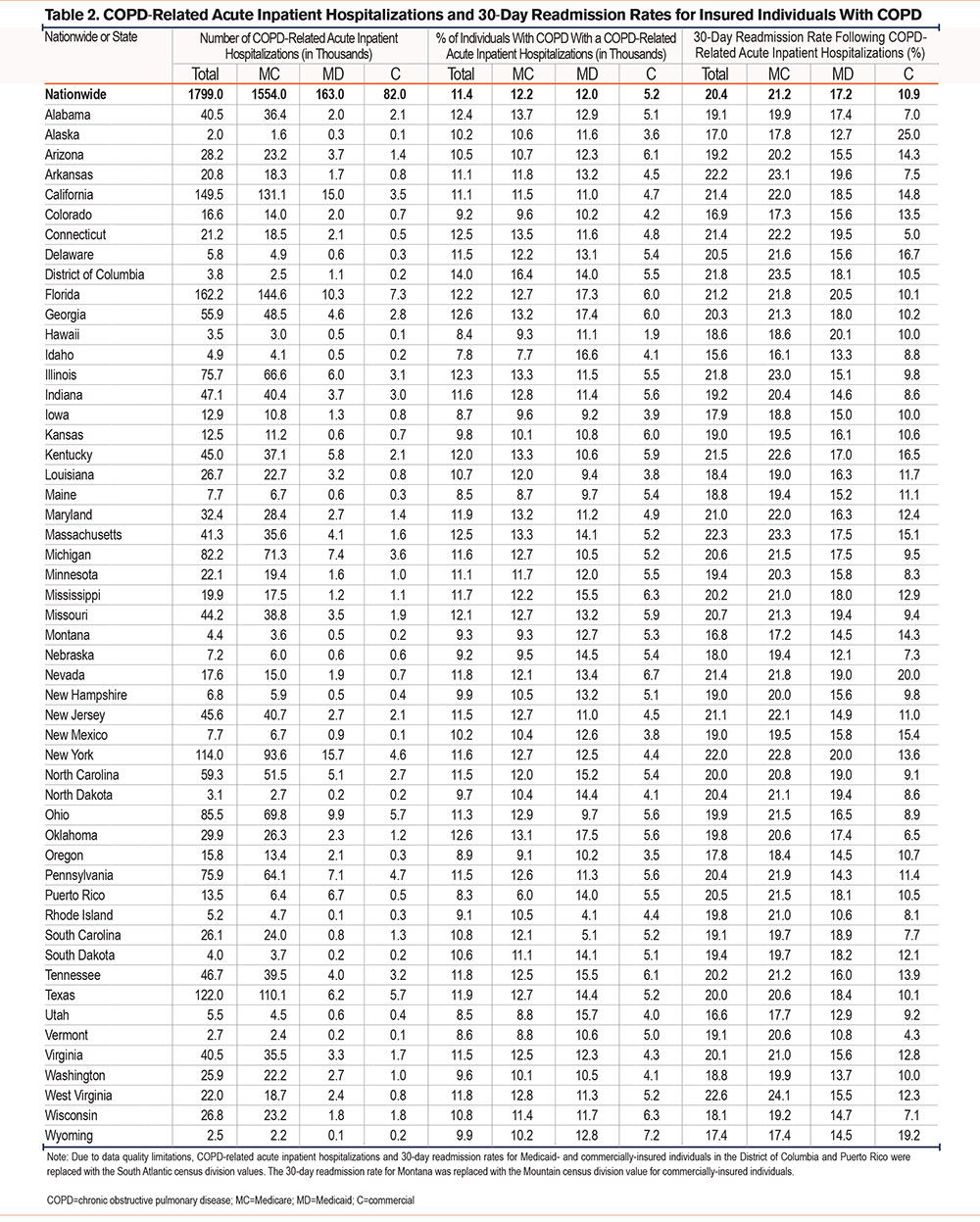
Figure 6 displays the 30-day all-cause readmission rates following COPD-related acute inpatient hospitalizations by insurance type and state. Nationwide, readmission rates were highest in Medicare (21.2%), followed by Medicaid (17.2%) and commercial insurance (10.9%). Rates showed variability across states, with Medicaid (10.6% in Rhode Island to 20.5% in Florida) and commercial insurance (4.3% in Vermont to 25% in Alaska) showing wider variation than Medicare (16.1% in Idaho to 24.1% in West Virginia).
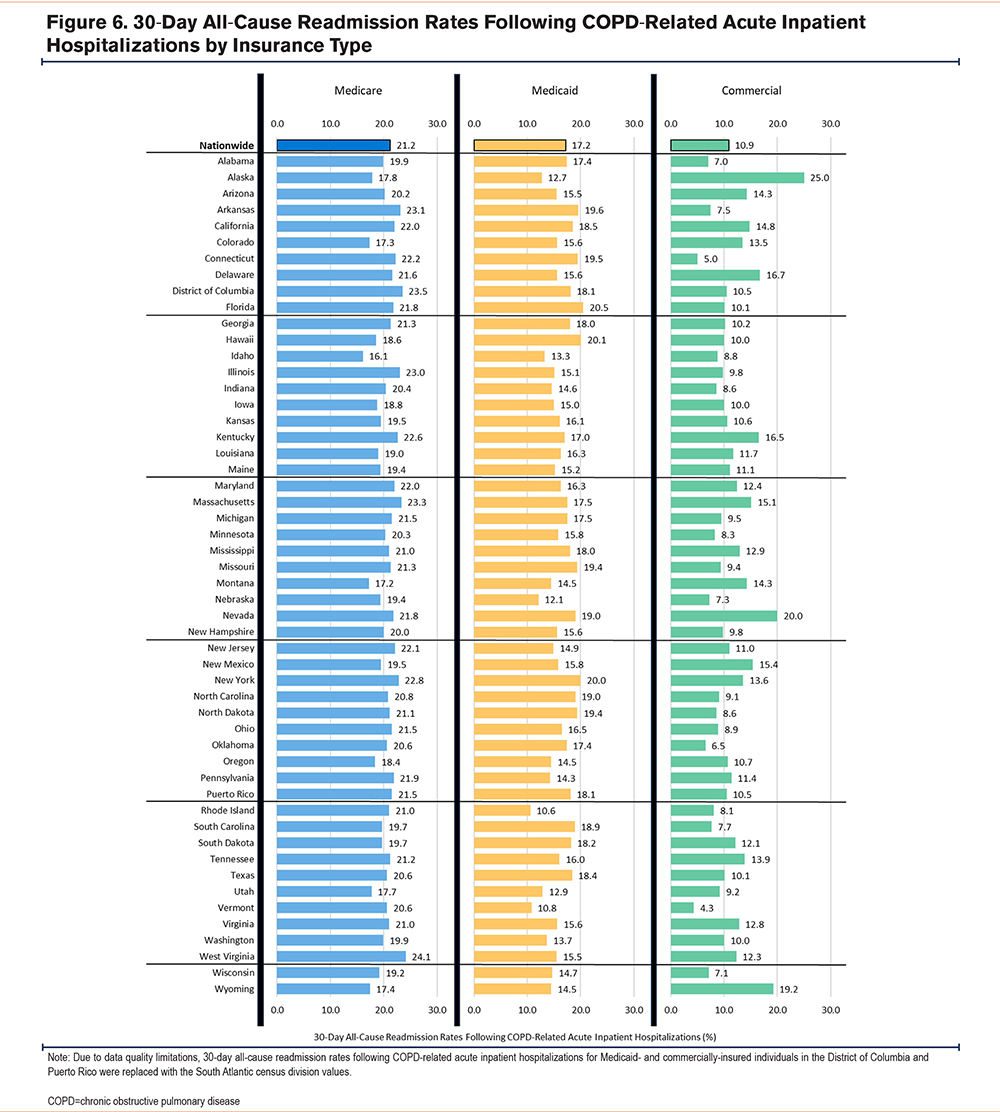
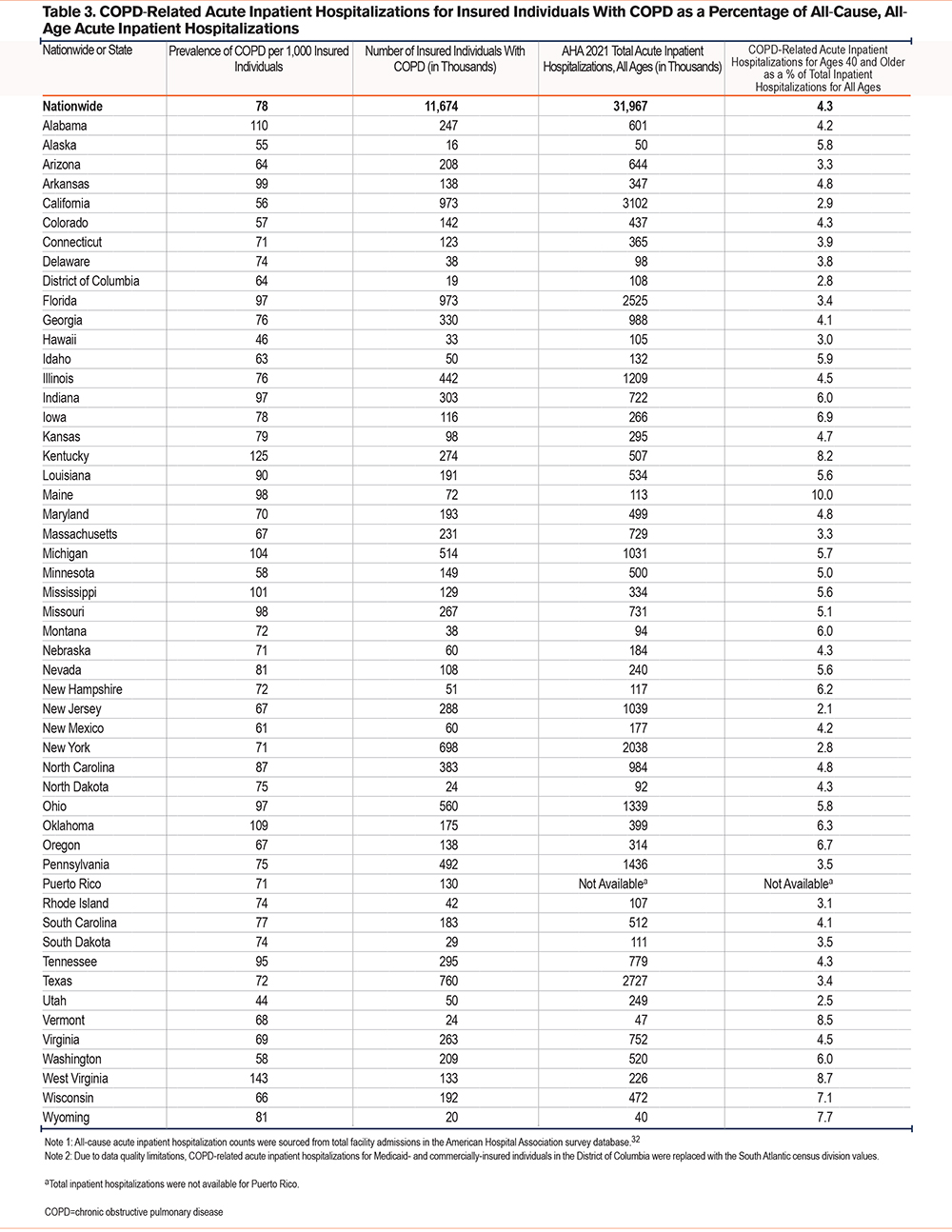
Table 3 displays the prevalence of COPD in insured individuals and shows the relationship between COPD-related acute inpatient hospitalizations for individuals aged 40 and older and all acute inpatient hospitalizations by state.32 Nationwide, COPD-related acute inpatient hospitalizations in insured individuals aged 40 and older accounted for 4.3% of all-cause hospitalizations for all ages nationwide. This percentage varied substantially across states, with the highest percentage seen in Maine (10.0%) and the lowest in New Jersey (2.1%). No adjustments were made for differences in the prevalence of COPD, demographic characteristics of states’ overall populations, Medicaid expansion experience, health care treatment patterns, or other unobserved factors.
Discussion
COPD is a major cause of morbidity and mortality in the United States, resulting in substantial disease burden that varies by state and health insurance type. Based on this analysis of administrative claims data, an estimated 11.7 million insured individuals, or 7.7% of the 40 and older U.S. population who were covered by insurance, had COPD in 2021. The annual all-cause mortality rate was 11.5% for individuals insured by Medicare and 5.1% for those insured by Medicaid. Furthermore, there were 1.8 million COPD-related acute inpatient hospitalizations in 2021, accounting for 4.3% of all acute inpatient hospitalizations in that year.
State-level COPD prevalence in this study varied widely, likely driven in part by differences in the state distribution of known risk factors for developing COPD (e.g., smoking). For example, West Virginia and Kentucky had the highest prevalence of COPD in insured individuals and the fifth-highest and highest rates, respectively, of current smoking among adults aged 45 and older in 2021.3 The state-level claims-based COPD prevalences in this study were directionally aligned with the survey-based prevalence estimates based on 2021 BRFSS data,3 although the claims-based rates were generally lower (e.g., West Virginia’s COPD prevalence in this study was 14.3% compared to 17.3% in BRFSS). This is consistent with other research comparing the prevalence of chronic conditions based on self-reported data (e.g., BRFSS survey data) to administrative claims estimates. Other studies have identified substantial differences in prevalence depending on the estimation methodology, potentially due to survey interpretation issues, selection into insurance and plan selection among insured individuals (e.g., FFS versus Medicare Advantage), and the stringency and specificity of claims-based disease identification algorithms.33
The burden of COPD varied among populations with different insurance types and within an insurance type across geography, especially for Medicaid where eligibility criteria varied across states. While commercial insurance covered the largest share (48.8%) of individuals, only 11.3% of individuals with COPD had commercial insurance. In contrast, Medicare’s share of individuals was lower at 41.0%, while its portion of insured individuals with COPD was much higher at 79.4%. The concentration of individuals with COPD in the Medicare-insured population is consistent with increasing age as a risk factor for COPD (Medicare’s average age is 73, compared to 56 in commercial insurance), as the disease can result from an accumulation of gene-environment interactions that cause persistent and progressive damage to the lungs over an individual’s lifetime.34 Medicaid insured only 9.3% of individuals with COPD despite a COPD prevalence 3 times the commercial rate, in part due to Medicaid insuring the lowest share (10.2%) of individuals.
State also played a role in the distribution of insured individuals, particularly Medicaid. While Medicare and commercial insurance eligibility criteria were generally consistent across states, Medicaid eligibility varied substantially across states that make local decisions (above a minimum threshold) about eligibility for Medicaid coverage. Compared to states that expanded Medicaid coverage prior to 2021, states that had not expanded Medicaid eligibility as of January 1, 2021, (except for Wisconsin) had higher COPD prevalence and lower proportions of individuals aged 40 to 64 who were insured by Medicaid. Future research using interrupted time-series design could analyze whether the more stringent low-income requirements in non-expansion states was related to Medicaid-insured populations being at higher risk of developing COPD.
All-cause mortality rates for individuals with COPD insured by Medicare or Medicaid varied by geography, although Medicare-insured individuals had consistently higher all-cause mortality than those insured by Medicaid. The higher age of the Medicare-insured population compared to the Medicaid-insured population (73 versus 55) likely contributed to this difference. However, within the Medicare-insured COPD population, the relationship between all-cause mortality and age was inconsistent across states. States with Medicare-insured COPD populations older than the national Medicare average did not consistently have higher all-cause mortality rates, nor did states with Medicare-insured COPD populations younger than the national average always have lower all-cause mortality. Of greatest public health concern were the 13 states (West Virginia, Kentucky, the District of Columbia, Mississippi, Oklahoma, Alabama, Maine, Louisiana, Arkansas, Indiana, Ohio, Tennessee, and Georgia) with lower-than-average ages but higher-than-average all-cause mortality rates for the Medicare-insured COPD population, where improved management of COPD and comorbid conditions may have the greatest opportunity to impact mortality. For example, COPD exacerbations may increase the risk of both respiratory and cardiovascular events that can lead to premature death.35 Moreover, states with dual-eligibility at or above the 75th percentile nationally were disproportionately more likely to have lower-than-average Medicare-insured ages but higher-than-average all-cause mortality rates. This finding suggests potential differences in risk factors for COPD exacerbations and comorbid conditions, including gaps in optimal management of COPD and other medical conditions in low-income Medicare-insured individuals with COPD in these states. This presents an opportunity for research into state-level COPD risk factors and treatment patterns, such as differences in air quality, smoking rates, obesity prevalence, adherence to Global initiative for chronic Obstructive Lung Disease (GOLD) 2024 COPD treatment guidelines,36 and access to specialty care. For example, among individuals with a history of severe COPD exacerbations, GOLD 2024 recommends dual bronchodilator treatment with a long-acting beta2-agonist (LABA) and a long-acting muscarinic antagonist (LAMA) or triple therapy with LABAs, LAMAs, and inhaled corticosteroids.36 Delays in initiation of triple therapy among individuals with severe COPD exacerbations are associated with an increased risk of exacerbations.37
COPD-related acute inpatient hospitalizations and 30-day all-cause readmissions following hospitalizations also showed variability by state and insurance type. COPD-related acute inpatient hospitalizations ranged from 97 (Idaho) to 200 (District of Columbia) per 1000 insured individuals with COPD, while 30-day all-cause readmission rates ranged from 15.6% (Idaho) to 22.6% (West Virginia). Other research has shown that 55% of readmissions following COPD-related hospitalizations were attributable to non-COPD conditions at the time of return,38 highlighting the importance of timely follow-up and effective care management of COPD and other medical conditions during transition from the hospital to the community when the risk of adverse events is high.39 However, hospitalization and readmission rates alone did not fully represent the burden of COPD on the health care system, as the total number of insured individuals with COPD in each state substantially impacted the absolute number of COPD-related acute inpatient hospitalizations and readmissions. For example, the District of Columbia was among the states with the lowest number of COPD-related acute inpatient hospitalizations nationally despite having the highest hospitalization rate, owing to its smaller number of insured individuals with COPD. In all states except Puerto Rico, Medicare-insured individuals with COPD accounted for the highest share of COPD-related hospitalizations and readmissions. Furthermore, in most states, Medicaid-insured individuals accounted for a higher share of COPD-related hospitalizations and readmissions than commercially-insured individuals, even though Medicaid generally insured a lower percentage of individuals with COPD. This is consistent with research showing higher rates of acute inpatient hospitalizations for most chronic conditions among Medicaid-insured compared to commercially-insured individuals.40
This study has several limitations. The analysis used health insurance claims to identify and characterize individuals diagnosed with COPD and quantify COPD-related metrics. Differences and imprecision in coding practices could have resulted in over-identification or under-identification of insured individuals with COPD and COPD-related acute inpatient hospitalizations, and health care access barriers could contribute to under-identification. The study was limited to individuals insured by Medicaid, Medicare, and commercial insurance, excluding those with other insurance types and the uninsured population, which may have disproportionately impacted COPD-related metrics for certain states. Metrics for some states were replaced with regional values due to noncredible sample sizes and/or data quality limitations, and the results for those states could differ from the census division values reported (see Methods section). No adjustments were made for sex, gender, age, or underlying health differences across insurance types and states, so outcomes may reflect differences in population characteristics unrelated to COPD. In addition, information was insufficient to identify individuals who switched between commercial insurance and Medicare or Medicaid in 2021, so some individuals could have been represented in multiple insured populations. Lastly, the effects of the COVID-19 pandemic likely had an impact on the results of this study, including underestimation of COPD prevalence due to fewer opportunities for COPD diagnosis codes to be reported on claims,41 decreased COPD-related acute inpatient hospitalizations due to public health measures implemented during the COVID pandemic,42 and decreased rates of ED/Obs encounters and hospitalizations for minor COPD exacerbations due to patients avoiding the ED and the tightening of criteria for inpatient admission in order to preserve hospital bed capacity.43 In Medicaid, the continuous enrollment provision of the Families First Coronavirus Response Act44 also increased membership substantially during this period by maintaining insurance coverage for healthier individuals who may have lost Medicaid coverage in previous years. This would be expected to result in lower observed COPD prevalence and lower rates of COPD-related acute inpatient hospitalizations for individuals insured by Medicaid during this time period compared to the prepandemic period and the period after the unwinding of continuous Medicaid enrollment45 following March 2023. Analyses with different time periods, data sources, or methodologies would be expected to have different results.
Health insurance administrative claims are a robust and credible data source that can provide comprehensive information about insured individuals living with COPD. Taken together, the insurance types included in this study (Medicare, Medicaid, and commercial insurance) provide coverage for 90% of the U.S. population, with the remaining 10% either uninsured or covered under insurance types not included in this study (e.g., Veterans Administration).46 COPD is a treatable disease, but gaps in care remain resulting in underdiagnosis, misdiagnosis, and inadequate or inappropriate treatment that can lead to more frequent and more severe exacerbations.37 Understanding the variation in prevalence, demographics, and acute hospital-based utilization of individuals with COPD by state and insurance type provides valuable insights into high-burden areas and population groups with unmet needs. This can be used to develop and refine public health strategies to address these gaps in order to reduce the burden of COPD on individuals and the health care system. Future hypothesis-driven research could expand this understanding by adjusting for underlying differences in the COPD population clinical and demographic characteristics across insurance types and states, allowing statistical comparisons of differences across various populations.
Acknowledgements
Author contributions: All authors contributed to the conception and design of the study, data analysis and interpretation, and drafting and revising the manuscript prior to submission. All authors gave final approval for this version of the manuscript to be published.
The authors would like to thank Amanda McCarthy, Ananya Sridharan, Ifrah Fayyaz, Jared Hirsch, Jaron Jackson, Swad Komanduri, Vivian Chen, and Yen Chung for their helpful contributions to the analyses, visuals, and supporting materials, as well as Jessica Naber for her review of this manuscript.
Declaration of Interest
CB, MA, SL, and WF are employees of Milliman, Inc., and received consulting fees from AstraZeneca. NF and HG are employees of AstraZeneca Pharmaceuticals LP and hold AstraZeneca stock. DM is a consultant to GlaxoSmithKline, AstraZeneca, Regeneron, Genentech, and the COPD Foundation and receives royalties from Up-to-Date and testifies on behalf of individuals suing the tobacco and vaping industries. The authors report no other conflicts of interest in this work.
This study was funded by AstraZeneca Pharmaceuticals LP (Wilmington, Delaware). Milliman, Inc., received consulting fees from AstraZeneca Pharmaceuticals LP to conduct the research and provide editorial support for the manuscript.